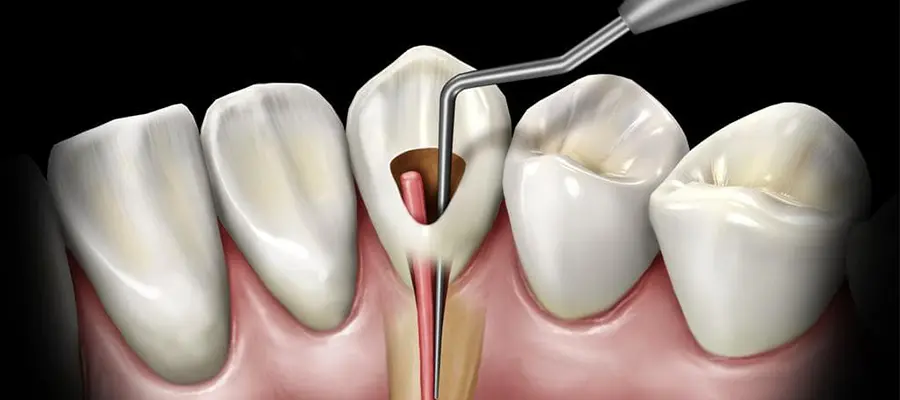
Endodontics is the branch of dentistry that aims to preserve the nerve and blood vessel tissue located inside the tooth. The most common procedure is root canal treatment. When a cavity progresses, a crack forms in the tooth, or pain develops after trauma, the inner tissue of the tooth can be affected. This may show itself as sensitivity to hot and cold, pain that increases at night, aching while chewing, and sometimes swelling.
The goal of endodontic treatment is to remove infected or damaged tissue and seal the canals with special filling materials. In this way, the tooth remains in the mouth and continues to function. Mild sensitivity may be seen for a few days after the procedure. Regular follow-ups and good oral care support the long-term success of the treatment.
What Is Endodontics?
Endodontics is the field of diagnosis and treatment related to the pulp tissue inside the tooth (nerve, blood vessels, and connective tissue). The role of this tissue is to keep the tooth alive and responsive to external factors. When decay deepens, a crack forms in the tooth, or the tooth is hit, the pulp may be affected. The main goal of endodontics is to correctly identify the source of pain and infection, restore the inner tissue of the tooth to a healthy state, and, if possible, keep the tooth in the mouth.
The most common endodontic procedure is root canal treatment. Root canal treatment helps protect the tooth without extraction and aims to maintain chewing function. In successful endodontic care, cleaning the canals thoroughly and filling them in a leak-proof way is important so the infection does not return. Good oral care after treatment, regular check-ups, and following your dentist’s instructions support the tooth staying problem-free for a long time.
When Is Endodontics Needed? What Is Root Canal Treatment?
Endodontics may be needed when the inner tissue of the tooth becomes inflamed or is affected in a way that cannot be reversed. Long-lasting sensitivity to hot and cold, throbbing pain that increases at night, aching that starts on its own, a sharp feeling while chewing, pain when biting down, and sometimes swelling in the face or gums may indicate the need for an endodontic evaluation. Teeth with deep cavities, cavities developing under old fillings or crowns, and teeth that show color change after trauma can also be candidates for root canal treatment. In some cases, even without obvious pain, an infection at the root tip may be detected and treatment can be planned.
Root canal treatment is a procedure designed to protect the tooth without extraction when the pulp tissue is damaged or infected. The basic logic is to remove infected or non-vital tissue from inside the tooth, clean the canals, and then seal the canals with filling materials. This helps control the infection spreading toward the root tip, reduces pain, and allows the tooth to remain in the mouth. Root canal treatment is often seen as a tooth-saving option, but the condition of the tooth’s upper structure and additional problems such as cracks can affect the treatment plan.
How Is Root Canal Treatment Done?
The procedure usually starts with an examination and an X-ray. The X-ray helps assess the root anatomy, the number of canals, and whether there is a problem around the root tip. Then the tooth is numbed, and the tooth is isolated to keep the area clean during treatment. A small access opening is made to reach the canals. At this stage, the canal length is measured and the goal is to prepare the canals to the correct working length. The aim is to remove infected tissue and shape the canal so it can be properly filled.
The canals are cleaned, shaped, and disinfected using special hand instruments or rotary systems and irrigation solutions. After cleaning is completed, the canals are filled in a leak-proof way and the upper part of the tooth is sealed with a filling. If the tooth has significant structure loss, a crown may be recommended to reduce the risk of fracture. Mild pain or sensitivity may occur in the first days after the procedure, and this is often related to tissue healing. If severe pain, increasing swelling, or noticeable pain while biting continues, planning a follow-up visit is appropriate.
Which Teeth Can Endodontics Be Applied To?
Endodontics can be applied to any tooth whose pulp tissue is affected. All teeth that have root canals, including front teeth, premolars, and molars, can be candidates for endodontic treatment. In front teeth, the number of canals is usually lower, and complaints are often seen as pain or color change after trauma. In molars, deep decay, problems under old fillings, and pain during chewing are among the more common causes.
Whether the treatment can be done is closely related to how structurally sound the tooth is and the condition of the surrounding tissues. If there is an advanced fracture, a root crack, severe structure loss, or serious problems in the tissues supporting the tooth, the treatment plan may change. For this reason, the decision becomes clear with an examination and X-ray evaluation. The goal is always to choose the safest approach to keep the tooth in the mouth without extraction whenever possible.
How Long Does Endodontic Treatment Take?
The duration of endodontic treatment varies depending on the canal anatomy, the status of infection, and the type of procedure needed. A simple root canal treatment can often be completed in one visit. In teeth with fewer canals, the procedure is usually shorter. In multi-canal molars, finding, cleaning, and shaping the canals can take more time.
In some cases, more than one visit may be needed. Especially if there is an infection at the root tip, placing medication inside the canals and waiting for a period may be preferred. Retreatment of a previous root canal, calcified canals, curved root anatomy, or an abscess can also increase the number of visits. When planning treatment time, the goal is not to finish quickly, but to clean the canals well and seal them in a leak-proof manner.
Is Root Canal Treatment Painful?
With proper numbing, root canal treatment is generally not a painful procedure. Local anesthesia applied before the procedure largely removes pain sensation from the tooth and surrounding tissues. In people who have pulp inflammation due to decay, it is common to feel relief once treatment begins, because the goal is to remove the source of pain.
After the procedure, mild sensitivity, aching, or discomfort while biting may occur for a few days. This is often related to the healing process of the tissues around the root. The discomfort usually decreases over time. However, if there is severe pain, increasing swelling, fever, or a strong feeling that the bite is “too high,” a check-up is recommended. Following the pain relief and care guidance provided by the dentist helps make the process more comfortable.
What Should Be Considered After Endodontic Treatment?
➤Avoid eating until numbness wears off to reduce the risk of biting the cheek or tongue.
➤Avoid hard, very hot, and very cold foods during the first 24 hours.
➤For a few days, chewing less on the treated side helps reduce the load on the tooth.
➤If there is a filling or temporary filling, do not try to pull it off and avoid sticky foods.
➤If you have a habit of clenching or grinding, being more careful during this period is important.
➤Mild aching in the first days can be normal; if recommended, pain medication should be taken regularly.
➤Continue brushing and flossing to help keep the area clean.
➤If you feel the filling is “too high” or discomfort while biting continues, a check-up should be done.
➤If there is severe pain, increasing swelling, a bad taste or smell, or fever, an examination is needed without delay.
➤If the tooth has significant structure loss, a crown may be recommended, and appointments should not be delayed.
How Long Can a Tooth Last After Root Canal Treatment?
A tooth that has had root canal treatment can be used for many years without problems when restored with the correct filling or crown. In many cases, with regular care and follow-up, the tooth can remain in the mouth for life. Durability depends on factors such as structure loss, bite force, oral care, and the quality of the final restoration.
After root canal treatment, the main risks are tooth fracture and leakage around the restoration. Especially in back teeth with large cavities or big fillings, planning protection with a crown becomes more important. Regular brushing, flossing, and follow-up X-rays reduce the risk of new decay and make it easier to monitor the root tip area.
Differences Between Endodontics and Tooth Extraction
Endodontics aims to save the tooth without extraction. The inside of the tooth is cleaned and the root canals are filled to control infection. Because the natural tooth remains in the mouth, chewing sensation and bite balance are preserved. Also, since an extraction-related gap is avoided, issues such as shifting of neighboring teeth and over-eruption of the opposing tooth are less likely.
Tooth extraction is the complete removal of the tooth from the mouth, and the space often needs to be treated. If the space remains for a long time, chewing balance can be disrupted and tooth movement and bone loss can develop. Options after extraction include implants, bridges, or removable dentures, each with its own process and costs.
What Is Endodontic Retreatment?
Retreatment is the renewal of a root canal treatment when a tooth that previously had a root canal still has problems or develops a new infection. Causes can include a missed canal area, an inadequate canal filling, leakage under a filling or crown, decay that developed later, or a crack in the tooth. In some cases, even without symptoms, a problem at the root tip can be seen on an X-ray.
In retreatment, the old filling material is usually removed, the canals are cleaned again, and disinfected. Then the canals are filled again and the upper restoration is completed in a leak-proof way. Not every retreatment case is the same. The tooth anatomy, the condition of the previous work, and the health of tissues around the root guide the plan. In special situations, surgical procedures at the root tip may also be considered.
Endodontics Prices 2026
Endodontics prices in 2026 vary depending on the location of the tooth, the number of canals, the level of infection, and the complexity of the procedure. While the process can be shorter in front teeth, planning can differ in multi-canal back teeth because detailed cleaning and shaping are required. First-time root canal treatment and retreatment of a previously treated tooth are also not the same in terms of cost. For this reason, the most accurate approach is to clarify a personalized treatment plan after examination and X-ray evaluation.
In clinics, transparent pricing is often aimed for, and the scope of the entire process is explained clearly before treatment. After root canal treatment, a filling or a crown may be needed to strengthen the tooth, and these steps can affect the total budget. To clarify the process with a quick appointment, a detailed examination, and a treatment plan, you can contact us.
Frequently Asked Questions
Is endodontics the same as root canal treatment?
Endodontics is a specialty field, and root canal treatment is the most common procedure performed within this field. In other words, root canal treatment is part of endodontics. Endodontics covers diagnosis, treatment, and follow-up related to the inner tooth tissue and root canals. Besides root canal treatment, retreatment and certain advanced procedures are also included in this field.
Can a tooth hurt again after a root canal?
Yes, in some cases a tooth can hurt again after a root canal. Mild aching, sensitivity when biting, or pain when touched in the first days is often part of healing. However, if the pain increases over time, or if swelling or a bad taste or smell occurs, a check-up is needed. The cause can be leakage, new decay, a missed canal area, or a crack.
How many visits does a root canal take?
Many root canal treatments can be completed in one visit. In teeth with fewer canals, the process is usually shorter. In cases with infection, abscess, difficult canal anatomy, or retreatment, two or more visits may be planned. The number of visits becomes clear after examination and X-rays.
Is a crown necessary after a root canal?
A crown is not always necessary after every root canal, but it is strongly recommended for some teeth. Especially in back teeth with large cavities or big fillings, the tooth can become more prone to fracture. In such cases, a crown protects the tooth from the outside and increases durability. If structure loss is minimal, completing the tooth with a filling may be enough.
What happens if a root canal fails?
If a root canal fails, the first option is often endodontic retreatment. In this procedure, the old canal filling is removed, the canals are cleaned again, and refilled. In some cases, surgical treatment at the root tip may also be considered. If there is a crack or advanced structural loss, extraction and replacement options can be evaluated.
Can a root canal be done when there is a dental abscess?
Yes, a root canal can be done when there is an abscess, and it is often necessary. The goal is to remove the source of infection. If pain and swelling are very strong, drainage, canal medication, and additional treatments may be planned. In some cases, proceeding over multiple visits is preferred.
Can a tooth break after a root canal?
The risk of fracture can increase after a root canal because the tooth may have lost structure and can become more fragile over time. The risk is higher especially in back teeth and in teeth with large restorations. Bite adjustment, proper filling, and a crown when needed can reduce this risk. Clenching and grinding can also increase fracture risk.
What is the difference between an endodontist and a general dentist?
A general dentist performs overall diagnosis and treatment, while an endodontist has advanced training focused on root canals and the inner tooth tissue. Difficult canal anatomies, retreatments, and higher-risk cases are more often referred to an endodontist. In both approaches, the goal is to keep the tooth healthy and in the mouth. Which clinician to proceed with depends on the case.
When can you eat after a root canal?
It is recommended not to eat until numbness wears off. During numbness, the risk of biting the cheek or tongue increases and injuries may happen without noticing. If a temporary filling was placed, avoiding very hard and sticky foods on the first day is safer. If there is no special instruction from the dentist, you can start with soft foods once numbness has worn off.
Does a root canal-treated tooth change color?
Yes, color change can occur in some teeth after a root canal. This is more common in front teeth after trauma, in teeth that lost vitality, or due to older filling materials. If color change occurs, the tooth is evaluated and options such as internal bleaching may be planned if suitable. Regular follow-ups help manage the process for both aesthetics and health.